Sleep Disorders and Anxiety: Causes, Signs, and What Actually Helps

If you’ve ever lain awake at 2 a.m. — exhausted but unable to switch off, heart beating a little too fast, mind spinning through every worry and worst-case scenario — you already understand the painful overlap between sleep disorders and anxiety. Your body is begging for rest, but something inside won’t let it happen.
If that sounds familiar, you are not alone. The connection between sleep disorders and anxiety is one of the most misunderstood and most common struggles that people quietly carry. Millions of people in the United States and around the world live in this exact loop every single night. They can’t sleep because they’re anxious. And because they can’t sleep, their anxiety gets worse. And then they can’t sleep again.
This article is here to break that loop down, gently, honestly, and in a way that actually makes sense. Not with clinical distance or a list of facts you’ll forget by tomorrow. But with real understanding, practical tools, and the quiet reassurance that your struggles are real, valid, and something you can work through.
Let’s start from the beginning.
Table of Contents
What Are Sleep Disorders, Really?
A sleep disorder isn’t just having “a few bad nights.” We all have those. A sleep disorder is a persistent pattern that disrupts your ability to get the rest your body and mind deeply need.
Some of the most common sleep disorders include:
Insomnia is the most widely recognized. It means regularly struggling to fall asleep, stay asleep, or waking too early and not being able to drift back off. It can be short-term, triggered by stress or life changes, or long-term, lasting months or years.
Sleep Apnea is when your breathing repeatedly stops and starts during sleep. Many people don’t realize they have it. They just wake up feeling exhausted, no matter how long they were in bed. It’s particularly common in adults who snore or feel unrested after what should have been a full night’s rest.
Restless Leg Syndrome (RLS) creates an uncomfortable urge to move your legs, often at night, making it nearly impossible to settle into sleep.
Hypersomnia is excessive sleepiness during the day, even after sleeping through the night. It’s less talked about but just as disruptive.
Nightmare Disorder and REM Sleep Behavior Disorder involve disturbing or physically acted-out dreams that repeatedly jolt a person awake.
According to the American Sleep Association, over 50 to 70 million Americans suffer from a sleep disorder. That’s not a small number. That’s a quiet epidemic.
The Deep, Tangled Link Between Sleep Disorders and Anxiety
Here’s where things get really important to understand.
Sleep disorders and anxiety don’t just coexist. They actively feed each other in a cycle that can feel almost impossible to escape without the right understanding.
Think of it this way. When you’re anxious, your brain’s threat-detection system, called the amygdala, stays on high alert. Your nervous system doesn’t know the difference between a lion in the wild and a difficult conversation you have to have tomorrow. It just knows something feels dangerous. So it keeps you awake, ready, watching.
And when you’re sleep-deprived, the very part of your brain that helps you regulate emotions, called the prefrontal cortex, becomes less effective. So your anxious thoughts feel bigger. More threatening. Harder to reason your way out of.
The National Institute of Mental Health confirms that anxiety disorders are among the most common mental health conditions in the U.S., and poor sleep is both a symptom and a cause.
This is the loop. Anxiety disrupts sleep. Poor sleep amplifies anxiety. And around and around it goes, night after night, until it starts affecting your days too.
Real People, Real Nights: 5 Stories That Might Sound Like Yours
Sometimes the most helpful thing is simply to recognize yourself in someone else’s experience. So here are five relatable scenarios that many people dealing with sleep disorders and anxiety live through.
1. The Sunday Night Spiral
Maria is 32. She works in marketing and genuinely loves her job. But every Sunday night, without fail, she finds herself lying awake running through everything that could go wrong that week. A client presentation. A meeting she’s dreading. An email she should have sent on Friday. By the time her alarm goes off on Monday, she’s had maybe four hours of broken sleep and the anxiety she was dreading has already arrived.
2. The 3 A.M. Wake-Up
James is 45. He falls asleep fine. But somewhere around 3 a.m., his eyes open and his heart is pounding. He can’t pinpoint why. Nothing specific happened in a dream. He just wakes, wide-eyed, already tense, and then spends the next two hours lying there, trying to force himself back to sleep, which of course makes it worse.
3. The Student Who Can’t Switch Off
Priya is 21 and in her final year of college. She’s been dealing with what her friends just call “overthinking,” but lately it’s stopped her from sleeping most nights before anything important. Exams, deadlines, even social events she’s looking forward to trigger a night of barely sleeping. She’s started dreading going to bed.
4. The Parent Running on Empty
David is a father of two young children. He already doesn’t get enough sleep. But when he does get a quiet moment, he can’t stop his mind from running through everything he might be failing at. Is he a good enough parent? Are his kids okay? He lies awake in an exhausted but wired state that he doesn’t have a name for yet.
5. The Person Who Wakes Up Tired Every Single Morning
Sofia sleeps eight hours most nights. By all appearances, she’s doing everything right. But she wakes up feeling like she hasn’t slept at all. Heavy, foggy, emotionally flat. She’s starting to wonder if something is physically wrong with her, not realizing that her chronic anxiety is quietly fragmenting her sleep quality throughout the night, even when she doesn’t remember waking.
You might see yourself in one of these. Or in parts of all of them. What matters is knowing: this is not just “in your head.” It is real. And it has real solutions.
How Anxiety Physically Disrupts Your Sleep
Let’s get into what’s actually happening in your body when anxiety and sleep disorders collide.
When you experience anxiety, your body releases stress hormones, particularly cortisol and adrenaline. These hormones are brilliant for helping you respond to genuine danger. But when your brain perceives everyday worries as threats, they stay elevated longer than they should.
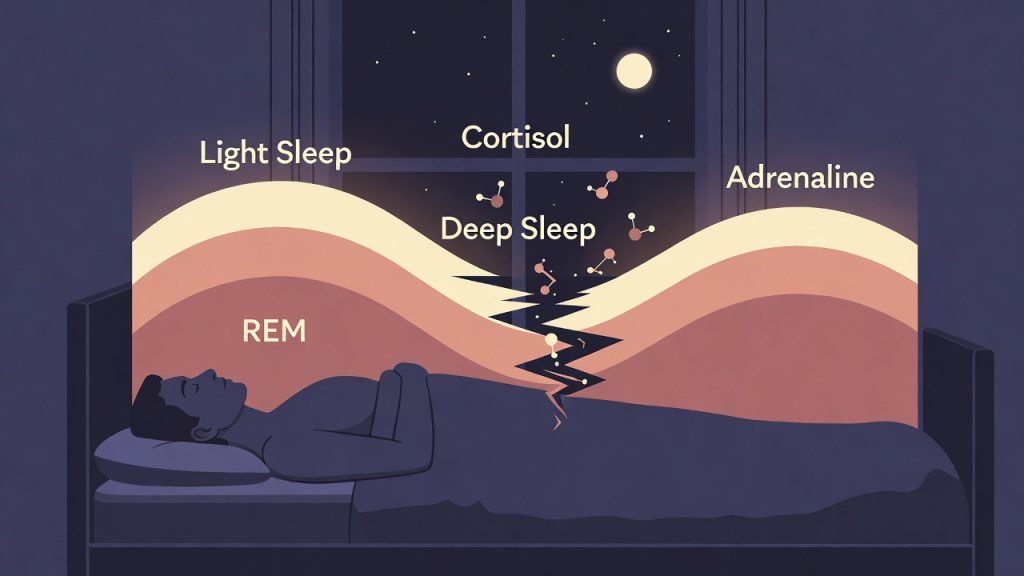
Elevated cortisol at night tells your body it needs to stay alert. Your heart rate rises slightly. Your breathing becomes shallower. Your muscles tense up, sometimes without you noticing. Your brain moves into a light, fragmented kind of sleep rather than the deep, restorative stages it needs.
Even if you spend eight hours in bed, anxiety can rob you of the slow-wave and REM sleep your brain needs to process emotions, consolidate memories, and genuinely recover. This is why so many people with anxiety wake up feeling exhausted even after a full night, a pattern that Mindbloom explores in depth in Why You Feel Exhausted Even After a Full Night’s Sleep.
The Sleep Foundation explains that approximately 24% to 36% of people with insomnia also have an anxiety disorder. The relationship runs in both directions, making treatment of either condition more complex without addressing both together.
Signs That Your Sleep Disorders and Anxiety Are Connected
Not every sleep struggle is anxiety-driven. But there are some telling signs that the two are connected for you specifically.
You might be dealing with anxiety-related sleep disruption if you notice that your sleep problems tend to worsen before stressful events, even ones you’re looking forward to. Or if your mind races the moment you lie down, running through worries, plans, or replayed conversations. Or if you wake in the early hours with a sense of dread or tension but no clear dream to explain it.
Other signs include grinding your teeth at night, waking with headaches or a tight jaw or clenched fists. Needing to check your phone or review your to-do list before you feel calm enough to sleep. Feeling like you can never fully “switch off,” even when you’re physically exhausted.
If rest never feels truly restful for you, even after long sleep, there is usually something worth exploring. The Mindbloom piece on why rest doesn’t always feel restful goes deeper into why rest doesn’t always do what it’s supposed to and what you can do about it.
Effective Treatments for Sleep Disorders and Anxiety
Here is some genuinely good news. Both sleep disorders and anxiety are highly treatable. You do not have to white-knuckle your way through every night forever.
Cognitive Behavioral Therapy for Insomnia (CBT-I)
CBT-I is widely considered the gold-standard treatment for chronic insomnia, and it works particularly well when anxiety is part of the picture. It’s a structured approach that helps you identify and change the thoughts and behaviors that prevent restful sleep. It’s not just about relaxation. It actively rewires how your brain relates to bedtime. The American Psychological Association has extensive resources on how and why it works so well.
Therapy for Anxiety
Working with a therapist, whether through cognitive behavioral therapy, acceptance and commitment therapy, or another approach, can significantly reduce the anxiety that is disrupting your sleep. Addressing the root of the worry takes pressure off the nights. If you’re wondering where to even start with professional support, the Mindbloom guide on what therapy really is and what to expect before you begin is a warm, honest place to begin.
Medication (When Appropriate)
For some people, medication is a genuinely helpful part of the picture. Sleep aids, anti-anxiety medications, or antidepressants that help with both can be prescribed by a doctor or psychiatrist. This is not a weakness. It is one tool in a larger toolkit. Always work with a healthcare provider to find what’s right for you.
Mindfulness and Relaxation Practices
Research supports the use of mindfulness meditation, progressive muscle relaxation, and deep breathing as tools that calm the nervous system and make sleep more accessible. These aren’t magic cures. But consistent practice genuinely changes how your body and brain respond to stress over time.
8 Practical Ways to Manage Sleep Disorders and Anxiety Starting Tonight
You don’t have to wait for a diagnosis or a therapy appointment to begin making things better. Here are eight evidence-informed steps you can take starting right now.
1. Set a consistent sleep and wake time. Even on weekends. Your body clock responds to routine more than you might think. Consistency trains your brain to wind down at the same time each night.
2. Create a wind-down ritual. Start at least 30 minutes before bed. Dim the lights, put your phone face down, and do something that genuinely calms you. Reading, stretching, a warm shower. Signal to your nervous system that the day is over.
3. Try the 4-7-8 breathing method. Inhale for 4 counts, hold for 7, exhale for 8. This activates your parasympathetic nervous system, the part that tells your body it’s safe to rest.
4. Write your worries down before bed. Keep a small notebook on your nightstand. If your mind starts racing, write it down and tell yourself: “I’ve noted it. I can think about it tomorrow.” This simple act helps your brain release the need to hold onto it overnight.
5. Limit caffeine after 2 p.m. Caffeine has a half-life of around 5 to 6 hours. That afternoon coffee is still very much in your system at 10 p.m.
6. Get out of bed if you’ve been awake for 20 minutes. This is a CBT-I strategy called stimulus control. Lying awake in bed for too long teaches your brain to associate bed with wakefulness and worry. Get up, do something calm in dim light, and return when you feel sleepy.
7. Reduce screen exposure an hour before bed. Blue light suppresses melatonin production. But equally important is the content: doom-scrolling, news, or emotionally activating social media all prime your nervous system for alertness at exactly the wrong time.
8. Try grounding techniques if you wake anxious in the night. The 5-4-3-2-1 technique, naming five things you can see, four you can feel, three you can hear, two you can smell, one you can taste, can interrupt an anxiety spiral and bring you back to the present. Mindbloom has a deeper look at simple grounding techniques you can use for anxiety that work in moments of real distress.
When to Reach Out for Professional Help
There is a point where trying to manage this alone is no longer the right approach. And recognizing that point is not failure. It’s wisdom.
Consider speaking to a doctor or mental health professional if any of the following apply: your sleep problems have persisted for more than a few weeks; daytime functioning is seriously affected; you’re experiencing panic attacks, persistent dread, or a fear of going to bed; you suspect you might have sleep apnea or another physical sleep condition; or your mental health is declining in ways that feel beyond what self-help can address.
According to the Centers for Disease Control and Prevention, adults need at least 7 hours of quality sleep per night for optimal health — and about 1 in 3 American adults report not getting enough. If you are consistently falling far short of that, that is a health issue that deserves professional attention, not just more willpower.
Asking for help is one of the bravest, most self-compassionate things you can do. If you’re unsure whether what you’re experiencing is “serious enough” for therapy, the Mindbloom article on knowing when to see a therapist can gently help you find that answer.
You Can Break the Sleep Disorders and Anxiety Cycle
The relationship between sleep disorders and anxiety is real, clinically recognized, and something that millions of people navigate every single night — often without knowing that effective help exists. But understanding it is already the beginning of changing it.
You deserve to sleep. Not as a reward for doing everything right. Not once the worry disappears or the to-do list clears. Right now, as you are, with everything you are carrying.
Rest is not a luxury. It is not laziness. It is the foundation from which everything else in your life grows. And you are worth the effort it takes to protect it.
Be patient with yourself. Small steps taken consistently will change your nights. And slowly, they will change your days too. Your brain is not broken. Your body is not failing you. You are simply asking for the rest you have always deserved.
Start there. Tonight.

Frequently Asked Questions About Sleep Disorders and Anxiety
1. Can anxiety cause sleep disorders? Yes, absolutely. Anxiety is one of the most common causes of insomnia and other sleep disturbances. Chronic anxiety keeps the nervous system in a heightened state of alertness, making it difficult to fall asleep, stay asleep, or reach the deeper, restorative stages of sleep your body truly needs.
2. What is the most common sleep disorder linked to anxiety? Insomnia is the sleep disorder most frequently linked to anxiety. People with generalized anxiety disorder, social anxiety, and panic disorder are significantly more likely to experience chronic insomnia than the general population.
3. How do I know if my insomnia is caused by anxiety? If your sleep problems worsen during stressful periods, if your mind races at bedtime with worries or replayed conversations, or if you regularly wake in the early hours with a sense of dread, anxiety is likely playing a role. A doctor or therapist can help with a proper assessment.
4. Does treating anxiety improve sleep? In most cases, yes. When anxiety is managed effectively through therapy, lifestyle changes, or medication, sleep quality tends to improve alongside it. The two are so deeply interconnected that improving one almost always supports the other.
5. What helps with anxiety-related insomnia specifically? Cognitive Behavioral Therapy for Insomnia (CBT-I) is the most evidence-supported treatment available. Mindfulness practices, consistent sleep schedules, bedtime wind-down routines, and journaling also significantly reduce anxiety’s impact on sleep quality.
6. Is it normal to wake up anxious in the middle of the night? It’s common, but it isn’t something you simply have to live with. Waking with anxiety, particularly between 2 a.m. and 4 a.m., is often linked to the body’s natural cortisol rise in the early morning hours, which anxiety significantly amplifies. Therapy, stress management, and healthy sleep habits can reduce this pattern over time.
7. Can sleep deprivation make anxiety worse? Yes. This is one of the key reasons the cycle is so difficult to break. Sleep deprivation impairs the prefrontal cortex, the part of the brain that helps regulate emotions and rational thought. When this area is underperforming, anxious thoughts feel larger, more urgent, and harder to manage.
8. What is the “3 a.m. anxiety wake-up”? The “3 a.m. anxiety wake-up” is a widely recognized pattern where people with anxiety routinely wake in the early morning hours with racing thoughts or a sense of dread. It is connected to the body’s natural cortisol rise in the early morning, which anxiety amplifies considerably beyond what is helpful.
9. Are there natural remedies for sleep disorders and anxiety? Some natural approaches have limited research support, including magnesium, valerian root, chamomile tea, and lavender aromatherapy. Mindfulness practice is among the more consistently supported options. It’s important to speak with a doctor before adding any supplement to your routine, especially if you take other medications. These approaches work best as complements to evidence-based care, not replacements for it.
10. When should I see a doctor about my sleep problems and anxiety? If sleep problems persist for more than three to four weeks, significantly affect your ability to function during the day, or are accompanied by symptoms of depression, panic attacks, or other mental health concerns, it is time to speak with a doctor or mental health professional. Early support leads to considerably better outcomes.
Disclaimer
The content in this article is written for informational and educational purposes only. It is based on general wellness knowledge and is not intended to serve as medical advice, diagnosis, or treatment. Mindbloom is a personal blog, not a clinical resource. Always consult a qualified healthcare provider or licensed mental health professional for advice that is specific to your situation. If you are in crisis, please contact a helpline in your area. You can find one at befrienders.org.

